
Dr Shahid Jameel is a noted Indian virologist popularly known for his research in Hepatitis E virus. He is an elected fellow of all the three major Indian science academies viz. National Academy of Sciences, India, Indian Academy of Sciences, and Indian National Science Academy. The Council of Scientific and Industrial Research, the apex agency of the Government of India for scientific research, awarded him the Shanti Swarup Bhatnagar Prize for Science and Technology, one of the highest Indian science awards for his contributions to Medical Sciences in 2000. Here is an excerpt from Dr Shahid Jameel‘s interview:

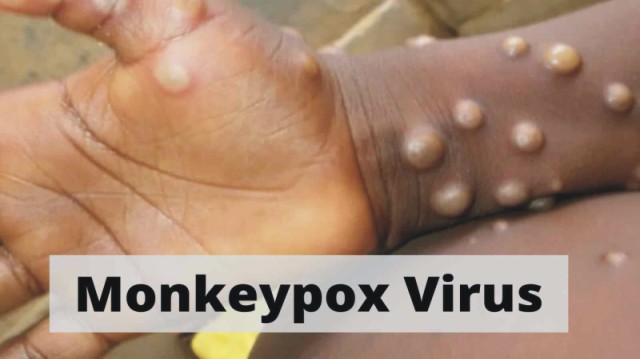
The Monkeypox and Covid-19 viruses are completely different. They belong to different families of viruses. Poxviruses are the largest (size 200-400 nm) and most complex animal viruses with DNA as their genetic material (average size about 200 kilobases). Coronaviruses are simple animal viruses (size about 100 nm) with RNA as their genetic material (average size about 30 kilobases).
Being DNA viruses, poxviruses have stable genomes while coronaviruses being RNA viruses can change quickly – as seen with so many variants of the Covid-19 virus.
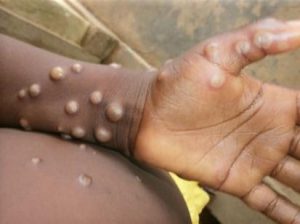
The two viruses also cause completely different disease manifestations – poxviruses produce skin boils; the Covid-19 virus produces a respiratory infection. This has implications for how the two viruses are transmitted from an infected to naïve host.
On the face of it, with few known cases in India at this time, the threat is small. But these cases (and those globally) are based not on community surveillance but were found in those who sought medical help. The actual numbers may be much higher everywhere in the world for us to be able to see over 17,000 known cases globally.
For India, I would say it’s not a cause for worry at this time but can quickly become one. So we need to be vigilant and put various public health measures in place.
No, we should not make that mistake. Though Monkeypox transmits mainly through touching and among close contacts, it also spreads through body fluids and droplets (i.e. surface contamination). Such infections can spread very quickly in places with high population density. Indian cities are crowded and come in that category.
The key lessons from Covid-19 are to recognise the problem early, not be complacent, put in public health measures (testing, isolation and treatment) early, communicate clearly, use the best tools available and use data to set policy. All these apply to Monkeypox as well.
India’s strength is not in vaccine development but in manufacturing. We can leverage that strength to license and produce large amounts of the available third generation smallpox vaccine (which is approved for use against Monkeypox as well). Research into new vaccines and bringing them to the market will take time. It will also be hard for the world to come up again with the kind of capital it did for Covid-119 vaccines, especially since most economies have been adversely affected by the ongoing pandemic.
So far I would say yes because the reported numbers are low. But since this has the potential to spread quickly, we should have a clear and coordinated plan. The Ministry of Health and Family Welfare, Govt of India issued guidelines for Monkeypox management in the country on 31st May 2022 even before any case was detected. This is a very good step.
Going beyond the guidelines issued well ahead of time, the key elements of preparedness would be testing, tracing, isolation and treatment.
 Increase testing facilities beyond NIV, Pune. During Covid-19, multiple laboratories across the country developed PCR testing capability. ICMR has set up Virology units in over 50 medical colleges. Training in containment and testing can increase their capabilities and quickly expand testing. NIV can play a trainer and quality control role.
Increase testing facilities beyond NIV, Pune. During Covid-19, multiple laboratories across the country developed PCR testing capability. ICMR has set up Virology units in over 50 medical colleges. Training in containment and testing can increase their capabilities and quickly expand testing. NIV can play a trainer and quality control role.
Testing sewage water for Monkeypox (like successfully done for Covid-19) can be implemented for cities that have the highest risk due to high population density. Cities also have a working sewage system (unlike villages). Virus in sewage is a good indicator of community transmission. This can guide public health planners and help fine tune the response.
Use India’s vaccine manufacturing strength to license and manufacture the Bavarian Nordic vaccine for India and other LMICs.
Use India’s generic pharma industry, to license and manufacture the FDA approved drug Tecovirimat for India and other LMICs.
The most important preparation for future is a robust and well-funded infectious disease research programme in the country. Viruses appear to be emerging at increased frequency. We can only keep ahead of them through research.
___________
Also Read:
Centre’s Opaque Auction Rules For Pulses Rip Off Govt Coffers, Help Millers Strike Rich
Need to amend laws like UAPA to provide for punishment for those who slap false cases
Global Arms Trade: Who are the real winners?
Why not 40 pc tickets for women in Punjab and elsewhere?
Punjab – How a deadly cocktail of Agri-Water-Energy nexus going to destroy it?

Disclaimer : PunjabTodayTV.com and other platforms of the Punjab Today group strive to include views and opinions from across the entire spectrum, but by no means do we agree with everything we publish. Our efforts and editorial choices consistently underscore our authors’ right to the freedom of speech. However, it should be clear to all readers that individual authors are responsible for the information, ideas or opinions in their articles, and very often, these do not reflect the views of PunjabTodayTV.com or other platforms of the group. Punjab Today does not assume any responsibility or liability for the views of authors whose work appears here.
Punjab Today believes in serious, engaging, narrative journalism at a time when mainstream media houses seem to have given up on long-form writing and news television has blurred or altogether erased the lines between news and slapstick entertainment. We at Punjab Today believe that readers such as yourself appreciate cerebral journalism, and would like you to hold us against the best international industry standards. Brickbats are welcome even more than bouquets, though an occasional pat on the back is always encouraging. Good journalism can be a lifeline in these uncertain times worldwide. You can support us in myriad ways. To begin with, by spreading word about us and forwarding this reportage. Stay engaged.
— Team PT

Copyright © Punjab Today TV : All right Reserve 2016 - 2024 |